
Arthrosis of the ankle joint — degenerative-dystrophic damage to cartilage tissue. But since as the disease progresses, the articular surfaces of the bones are involved in the process, it is more correct to call it osteoarthritis. In foreign literature, when describing this disease, the term osteoarthritis is used, which indicates not only degenerative changes, but inflammation against this background.
Osteoarthritis — This is a chronic, progressive joint disease in which cartilage, articular surfaces of bones, capsule and periarticular tissues are destroyed. This leads to pain and impaired joint mobility. The ankle rarely experiences osteoarthritis, unlike the knee. The disease occurs more often in women over 50 years of age and in athletes who have suffered foot injuries. For arthrosis of the ankle joint, treatment depends on the manifestations of the disease and is selected individually by an orthopedic traumatologist. Doctors use methods that have proven their effectiveness and safety, and practice a multidisciplinary approach to treating the problem and preventing the progression of joint pathology.
This article is advisory in nature. Treatment is prescribed by a specialist after consultation.
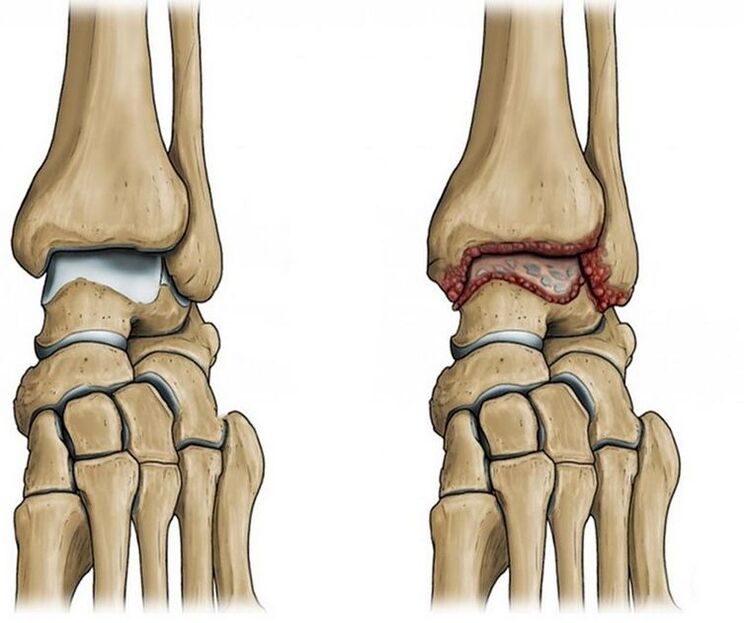
How the disease develops
The ankle joint is formed by three bones: the tibia, fibula and talus, covered with an articular capsule and strengthened by ligaments. Thanks to the work of the muscles, the foot bends and extends. Normally, the articular surfaces are smooth and easily slide relative to each other during movements. Covered with dense, elastic cartilage, its main function — bone protection and load absorption. The joint cavity contains synovial fluid. It plays the role of intra-articular lubrication, preventing friction of joint elements and their abrasion during movements.
But as a result of injury or natural aging of the joint, the articular surfaces become rough, and the cartilage tissue loses its smoothness and elasticity. When cartilage is damaged and as degenerative changes progress, the bones begin to come into contact with each other when moving in the joint, which is accompanied by pain.
In attempts to "defend"and to compensate for further damage to the joint and surrounding tissues, osteophytes are formed — growth along the edges of the articular surfaces of bones. As a result, the mobility of the joint is partially or even completely limited.
Depending on the root cause, the following types of osteoarthritis are distinguished:
- Primary or idiopathic osteoarthritis. In this case we are talking about degenerative-dystrophic changes in the joint
- Secondary is associated with exposure to a specific causative factor, usually a previous joint injury. And this form is most often diagnosed
Predisposing factors
The main predisposing factors for the development of arthrosis of the ankle joint:
- intra- and periarticular injuries, such as bone fractures, tears and ligament ruptures
- ankle surgery
- inflammatory joint lesions in the past
- intense loads: professional sports, ballet, long walking, work associated with long periods of being "on your feet"
- sedentary lifestyle
- wearing high heels for a long time
- excess weight
- hereditary collagenopathies leading to impaired collagen synthesis
- chronic injury to joint structures due to excessive loads
- metabolic disorders: diabetes, gout
- estrogen deficiency in postmenopausal women
- rheumatic diseases
- foot deformities, such as flat feet
- degenerative-dystrophic changes in the spine, complicated by the formation of an intervertebral hernia, which is accompanied by compression of the nerve root
Arthrosis of the ankle: symptoms
The main sign of arthrosis — Pain is what makes you seek help from a doctor. At the beginning of the development of the disease, the pain is bothersome only after prolonged exercise and decreases with rest.
Depending on the stage of pathological changes in the joint, the pain becomes more intense and persists at rest and even at night. Other symptoms occur.
There are three stages of the disease:
- The first stage is characterized by slight swelling, redness of the skin of the joint area, pain in the afternoon or after intense exercise. Unpleasant sensations are localized along the front surface of the foot, along the line of the joint and move to the lateral surfaces of the ankle. The x-ray of the foot may not yet show any changes.
- At the second stage, the pain becomes constant, a crunch appears when moving the joint, mobility is limited, and the joint "jams. "When examined on an x-ray, growths along the edges of the articular surfaces of the bones are noticeable: tibia, ankles and talus, as well as narrowing of the joint space
- At the third stage, the joint is deformed, which is why only rocking, low-amplitude movements are possible. The radiograph reveals massive bone growths, the joint space is sharply narrowed or even absent. Due to instability of the joint, patients often twist their leg, which only aggravates the situation due to sprains, tears of ligaments and deterioration of the general condition
Pain with ankle arthrosis has characteristic features:
- Maximum expressed at the beginning of movement — so-called starting pain
- Significantly increases with load, especially when running, jumping
- Often appears in the evening, at night or immediately after waking up
Due to pain, there is limited mobility of the foot, as well as jamming in the joint as the cartilage is destroyed.
Symptoms manifest themselves in waves: exacerbations alternate with remissions. With an exacerbation, the symptoms are more pronounced. During remission, the symptoms gradually subside and may even disappear altogether.
Which doctor should I contact?
If pain and stiffness in the movements of the ankle occur, you should consult an orthopedic traumatologist. If another cause of joint discomfort is identified, consultation with a neurologist, rheumatologist or endocrinologist may be required.
Diagnostics
To make a diagnosis, the doctor clarifies the complaints, specifies how long the pain has been observed, which contributes to its appearance and intensification. The specialist collects data on existing diseases, injuries and lifestyle characteristics, conducts an examination, assesses the range of motion in the joint and performs diagnostic tests.
Already on the basis of the information received, it is possible to assume a diagnosis, but to confirm it and draw up a competent treatment plan, additional examination methods are necessary, which may include:
- X-ray of the ankle joint, which is of primary importance in making a diagnosis and determining the stage of development of the disease. The images show narrowing of the joint space, osteophytes at the edges of the articular surfaces of the bones, cysts and signs of thinning of the bone located under the cartilage
- A CT scan of the joint reflects the picture in more detail. The doctor can assess in detail the condition of the patient’s bone structures and cartilage tissue
- MRI is used to study cartilage and soft tissues
- Ultrasound of the joint to assess the condition of soft joint structures
Treatment of arthrosis
Treatment of the pathology is long-term and is carried out under the supervision of an orthopedic traumatologist on an outpatient basis. How to cure arthrosis of the leg depends on the stage of damage and existing complications.
The main goals of treating the disease in a modern clinic are to relieve leg pain, improve the patient’s quality of life and slow down the progression of arthrosis. To do this, the doctor develops a set of therapeutic and preventive measures, medicinal and non-medicinal, and also adjusts the patient’s lifestyle.
Correction of lifestyle and nutrition
Sufficient physical activity and nutritional correction will help curb degenerative changes. After the examination, the clinic’s doctors can give recommendations on weight loss, as well as optimizing the load on the legs.
Drug treatment
Medicines are selected individually, based on examination data, symptoms, and concomitant diseases. The patient may be prescribed:
- Analgesics. Most often these are non-steroidal anti-inflammatory drugs in the form of tablets, gels, injections to relieve pain and inflammation
- Antidepressants and anticonvulsants for prolonged, severe, difficult-to-treat pain
Exercise therapy
Specially selected exercises help maintain range of motion in the joint, reduce pain, and curb the progression of degenerative changes. The patient performs the recommended exercises at first under the supervision of a specialist, and then — on your own, at home.
Massage
Massage of the lower limb normalizes nutrition of joint tissues. It is prescribed outside the acute stage. During the session, the specialist performs passive movements in the joint, which prevents muscle shortening and joint stiffness.
Assistive devices
Special orthoses, canes, and walkers may be recommended to relieve stress and stabilize the ankle joint.
Surgery
It is used only in cases of severe destruction of articular cartilage and limited joint mobility. After the operation there is a long period of rehabilitation and conservative treatment. Endoprosthetics or arthroplasty in the later stages of development of ankle arthrosis — practically the only opportunity to avoid disability and maintain joint mobility.
Why is ankle arthrosis dangerous?
Already formed changes in the joint are irreversible. Therefore, treatment is aimed at slowing down the pathological process in order to preserve the patient’s ability to work and quality of life. It is possible to achieve such goals only with timely treatment and strict adherence to the doctor’s recommendations.
As arthrosis develops, a pronounced deformation of the joint is formed. The range of movements sharply decreases, as a result, the ability to support the foot becomes difficult; walking without crutches or a cane is almost impossible.
Chronic, constant pain in the joint leads to anxiety and depressive disorders.
Prevention
Prevention of arthrosis includes the following measures:
- Avoid traumatic activities. For example, jumping from great heights, running
- Avoid injury
- Be careful in icy conditions, wear non-slip shoes
- Control your body weight
- Normalizing body weight will help reduce stress on the ankle joint
- Stay moderately active
- An inactive lifestyle is dangerous and leads to complications, as well as excessive overload and microtraumas
- Keep your joints healthy
- Consult a doctor promptly and treat musculoskeletal diseases
Main points from the article:
- The prevalence of degenerative-dystrophic diseases of the foot joints is 87%
- Occupational hazards, everyday habits, and past injuries can lead to arthrosis of the ankle joint.
- A common symptom of arthrosis — pain, which is accompanied by a crunching sound when moving, local swelling, and later limited mobility of the foot
- Treatment of ankle arthrosis is often conservative and includes both medicinal and non-medicinal methods.
- Progression of ankle arthrosis leads to disability and complete loss of foot function























